The immune system protects the body from harmful invaders (pathogens) and abnormal cells. It does this in two stages — a non-specific response (the same response to any pathogen, e.g. phagocytosis) and a specific response (involving lymphocytes, which target one particular pathogen).
Antigens
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
Each type of cell has specific molecules on its surface that identify it. These molecules include proteins and enable the immune system to identify:
- pathogens
- cells from other organisms of the same species
- abnormal body cells
- toxins.
Definition of antigen.
How does the body recognise a pathogen?
Every cell has specific molecules on its surface that act as identifiers — these are antigens. They can be proteins, glycoproteins, or glycolipids.
Antigens are how the immune system distinguishes self (own body cells) from non-self (foreign cells).
- Self antigens — on the body’s own cells; do not trigger an immune response
- Non-self antigens — on pathogens, transplanted cells, or abnormal body cells; do trigger an immune response
Antigens are used to detect:
- Pathogens — disease-causing organisms (bacteria, viruses, fungi)
- Cells from other organisms of the same species — important for organ transplant rejection
- Abnormal body cells — e.g. cancer cells, virus-infected cells
- Toxins — poisons (e.g. produced by some bacteria)
Definition
An antigen is a molecule (usually a protein) on the surface of a cell that triggers an immune response.
Antigen Variability
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
The effect of antigen variability on disease and disease prevention.
Some pathogens (e.g. influenza, HIV) have antigens that change frequently due to mutations in the genes that code for them. This is called antigen variability.
Effects on disease and prevention:
- Memory cells from a previous infection no longer recognise the new antigen. The immune system has to respond from scratch each time, so you can catch the same disease repeatedly (e.g. flu)
- Vaccines become ineffective — last year’s flu vaccine doesn’t protect against this year’s strain, as the antigens have changed.
- This is why we often need a new flu vaccine every year
Phagocytosis (Non-specific Response)
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
Phagocytosis of pathogens. The subsequent destruction of ingested pathogens by lysozymes.
Phagocytosis is the first line of defence against pathogens. It is non-specific — the same response happens to any pathogen. It’s carried out by phagocytes (a type of white blood cell).
- The phagocyte recognises non-self antigens on the pathogen and is attracted by chemicals released by the pathogen (chemotaxis)
- The phagocyte engulfs the pathogen by surrounding it with its cell-surface membrane, forming a vesicle called a phagosome
- A lysosome fuses with the phagosome
- Lysozymes (the hydrolytic enzymes inside the lysosome) hydrolyse / digest the pathogen
- The harmless products are absorbed by the phagocyte; some antigens are displayed on the phagocyte’s surface — it becomes an antigen-presenting cell (APC), which triggers the specific immune response
Don't confuse lysosomes with lysozymes
- Lysosome = the organelle (a membrane-bound vesicle containing enzymes)
- Lysozyme = the digestive enzyme inside the lysosome that breaks down the pathogen
Specific Immune Response
After phagocytosis (non-specific response) the body launches a specific response targeted at the particular pathogen. This includes:
- Cellular response — by T lymphocytes (T cells)
- Humoral response — by B lymphocytes (B cells) and antibodies
Both are triggered by antigen-presenting cells (APCs) - this is where the pathogen’s antigens are displayed on the APC’s surface.
Cellular Response (T Lymphocytes)
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
The response of T lymphocytes to a foreign antigen (the cellular response).
- The role of antigen-presenting cells in the cellular response.
- The role of helper T cells (T_H cells) in stimulating cytotoxic T cells (T_C cells), B cells and phagocytes. The role of other T cells is not required.
T lymphocytes mature in the thymus and respond to antigens displayed on Antigen Presenting Cells (APCs).
Cellular Response Process
- An antigen-presenting cell (e.g. a phagocyte, as we just looked at) displays the pathogen’s antigen on its surface. Note: This could be other antigen-presenting cells (e.g. cells infected by virus, cancer cells, foreign cells).
- A helper T cell with a complementary receptor binds to the antigen (clonal selection)
- This activates the helper T cell, which divides by mitosis (clonal expansion) — producing many identical helper T cells
- The activated helper T cells then stimulate:
- Cytotoxic T cells — these kill virus-infected cells and tumour cells (see below)
- B cells — to start the humoral response (see below)
- Phagocytes — to perform more phagocytosis
- Memory T cells — ready for a rapid response to any future infection by the same pathogen
- Note: For the AQA spec you don’t need to know the role of other T cells (e.g. regulatory T cells)
Cytotoxic T Cell
- These destroy abnormal (e.g. cancer cells) or infected cells
- They do this by releasing a protein called perforin
- This forms a pore in the cell-surface membrane, which allows cells and substances to freely enter and exit, and as a result the cell dies
Humoral Response (B Lymphocytes)
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
The response of B lymphocytes to a foreign antigen, clonal selection and the release of monoclonal antibodies (the humoral response).
B lymphocytes mature in the bone marrow. Each B cell has a unique antibody on its surface (a B cell receptor) that’s complementary to one specific antigen.
One B cell — one antibody specificity
Every B cell carries many identical antibodies on its surface — they all bind the same antigen. Different B cells carry different antibodies, so collectively the body has millions of B cells, each able to recognise a different antigen.
Humoral Response Process
- A B cell with the complementary receptor (this is the antibody on its surface) binds to the foreign antigen
- This is clonal selection - the antigen “selects” the B cell with the matching antibody
- The B cell takes in the antigen (internalises it), processes it, and presents it on its surface
- This is now an antigen-presenting cell (APC)
- A helper T cell binds to this same B cell (APC) and activates it
- (Extra detail ~ T helper cells release cytokines which activate the B cell)
- The activated B cell divides by mitosis
- This is clonal expansion - producing many identical clones of the selected B cell
- The clone of B cells differentiates into:
- Plasma cells — secrete large numbers of monoclonal antibodies (all identical, specific to the original antigen)
- Memory cells — stay in the blood long-term, ready for a rapid response to any future infection by the same pathogen
What is the difference between clonal selection and clonal expansion?
What is the difference between clonal selection and clonal expansion?
Easy to mix these up:
- Clonal selection = the antigen selects the B (or T) cell with the matching receptor. This happens at binding (step 1).
- Clonal expansion = the selected cell then divides by mitosis to produce many identical clones. This happens at step 4.
Think: select first, then expand. You can’t multiply a cell until you’ve picked the right one.
Antibodies
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
- Definition of antibody.
- Antibody structure.
- The formation of an antigen-antibody complex, leading to the destruction of the antigen, limited to agglutination and phagocytosis of bacterial cells.
All the monoclonal antibodies produced by the plasma cells are identical and bind to the same specific antigen on the pathogen, so they can be used by the immune system to destroy that specific pathogen.
Definition
An antibody is a protein (specifically, a quaternary-structure protein) produced by plasma cells that binds to a specific antigen.
Monoclonal means identical antibodies — produced from a single clone of plasma cells, so they all bind to the same specific antigen.
Antibody Structure
- Antibody is a quaternary protein - made of 4 polypeptide chains: 2 heavy and 2 light chains
- These chains are held together by disulfide bridges
- There are two identical variable regions, with the antigen-binding sites at the tips
- The variable region’s amino acid sequence is specific to one type of antigen — so one antibody can only bind to one type of antigen
- The rest of the molecule is the constant region (the same in all antibodies)
Why are antibodies important?
When an antibody binds to its specific antigen, they form an antigen-antibody complex. The pathogen is then destroyed in two ways:
- Agglutination — each antibody has two binding sites, so it can stick to two bacteria at the same time, acting as a bridge between them. Many antibodies doing this clump the bacteria together, making them too big to enter cells and easier for phagocytes to engulf
- Phagocytosis — the clumped pathogens are then engulfed and destroyed by phagocytes (as above)
Antibodies can also neutralise toxins released by bacteria — binding to the toxin prevents it from affecting cells.
Primary vs Secondary Immune Response
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
The roles of plasma cells and of memory cells in producing primary and secondary immune responses.
Your body reacts differently depending on whether it’s the first time a specific pathogen enters the body, or whether you have already encountered it before.
Primary Response (Slow, Fewer Antibodies)
- The first time the body meets a pathogen is called the primary response.
- It is generally slow, and creates only a few antibodies.
- Why? Because it has to go through the humoral response process, where the correct B cell needs to be selected (clonal selection) and then divide by mitosis (clonal expansion) to produce plasma cells, which can then produce antibodies. After this has happened, memory cells are produced.
- The person often shows symptoms of the disease.
Secondary Response (Faster, Lots of Antibodies)
- The next time the body meets the same pathogen is called the secondary response.
- It’s faster and creates lots of antibodies, often clearing the infection before symptoms appear.
- Because memory cells are already specific to the antigen and there are many of them, clonal selection is much faster — they recognise the antigen almost immediately, then divide rapidly into plasma cells.
| Primary response | Secondary response | |
|---|---|---|
| Speed | Slow (days) | Fast (hours) |
| Antibody concentration | Low | Much higher |
| Symptoms | Often experienced | Usually none |
| Why | First exposure — no memory cells yet | Memory cells divide rapidly into plasma cells |
Vaccination
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
The use of vaccines to provide protection for individuals and populations against disease. The concept of herd immunity.
A vaccine contains antigens from a pathogen in a form that can’t cause disease — usually a dead (inactivated) or weakened pathogen. The body responds as if it’s a real infection — producing a primary immune response, which produces memory cells.
If they later meet the real pathogen, they have a secondary immune response straight away, so don’t develop symptoms.
Herd Immunity
If a large enough proportion of the population is vaccinated, the pathogen can’t spread easily — even people who aren’t vaccinated are protected because they’re unlikely to come into contact with the pathogen.
This is important for:
- People who can’t be vaccinated (e.g. infants, the immunocompromised)
- Stopping outbreaks spreading through a population
Active vs Passive Immunity
What you need to know (based on the AQA specification)
What you need to know (based on the AQA specification)
The differences between active and passive immunity.
| Active immunity | Passive immunity | |
|---|---|---|
| How antibodies are made | The person’s own immune system produces them | Antibodies given from another source |
| Memory cells made? | Yes — long-term protection | No — only short-term protection |
| Speed of protection | Slow (takes time to produce antibodies) | Fast (antibodies are already present) |
Quick way to remember
- Active = active immune system (you do the work) → create memory cells, have long-term protection
- Passive = passive recipient (you’re given the antibodies), so have no memory cells, and only short-term protection
Can you name some examples of active vs passive immunity?
Can you name some examples of active vs passive immunity?
- Active immunity:
- Catching a disease naturally (e.g. chickenpox)
- Vaccination
- Passive immunity:
- Antibodies passed from mother to baby (across the placenta and in breast milk)
- Anti-venom / anti-toxin injections (e.g. for snake bites, tetanus)
Exam Question Practice
In Europe, viruses have infected a large number of frogs of different species. The viruses are closely related and all belong to the Ranavirus group. Previously, the viruses infected only one species of frog.
Suggest and explain how the viruses became able to infect other species of frog.
(2 marks)Hint
Think about how mutations change the shape of viral attachment proteins (antigens), and what that means for binding to host cells.
Mark Scheme
- Mutation in the viral DNA/RNA/genome/genetic material (1 mark)
- Altered (tertiary structure of the) viral attachment protein (1 mark)
- Allows it/attachment protein/virus to bind (to receptors of other species) (1 mark)
Tips from examiner reports
- Generic responses (“the virus mutates”) were not enough — the mutation must be linked to the virus evading the immune response
- Make sure to link mutation → changed antigen shape → existing antibodies no longer complementary
Describe how presentation of a virus antigen leads to the secretion of an antibody against this virus antigen.
(3 marks)Hint
Think helper T cell → B cell → clonal expansion → plasma cells.
Mark Scheme
- Helper T cell/TH cell binds to the antigen (on the antigen-presenting cell/phagocyte) (1 mark)
- This helper T/TH cell stimulates a specific B cell (1 mark)
- B cell clones OR B cell divides by mitosis (1 mark)
- (Forms) plasma cells that release antibodies (1 mark)
Comments from mark scheme
- “Helper” required once only
- Accept “This (helper) T cell stimulates a competent B cell” or “T cell stimulates B cell to undergo clonal selection” — this statement achieves both mp2 and mp3
Ranavirus is a virus that infects frogs.
Describe how the B lymphocytes of a frog would respond to vaccination against Ranavirus.
You can assume that the B lymphocytes of a frog respond in the same way as B lymphocytes of a human. Do not include details of the cellular response in your answer.
(3 marks)Hint
Stick to the humoral response only — receptor binding, clonal expansion, plasma cells, memory cells. No T cells.
Mark Scheme
- B cell (antibody) binds to (viral) specific/complementary receptor/antigen (1 mark)
- B cell clones OR B cell divides by mitosis (1 mark)
- Plasma cells release/produce (monoclonal) antibodies (against the virus) (1 mark)
- (B/plasma cells produce/develop) memory cells (1 mark)
Comments from mark scheme
- Accept “B cell forms antigen-antibody complex”
- Accept “B cell undergoes clonal selection/expansion”
Tips from examiner reports
- Common errors: not naming plasma cells specifically
- Some students made B cells become macrophages — wrong cell entirely
- Many included T cell responses despite being told not to — read the question’s restrictions carefully
Antivenom is produced by vaccinating animals with snake venom, so they produce antibodies against it. These antibodies are then extracted and used to treat snake-bite patients.
During vaccination, each animal is initially injected with a small volume of venom. Two weeks later, it is injected with a larger volume of venom.
Use your knowledge of the humoral immune response to explain this vaccination programme.
(3 marks)Hint
Why does the first dose need to be small? Why does the second dose work differently?
Mark Scheme
- B cells specific to the venom reproduce by mitosis (1 mark)
- (B cells produce) plasma cells and memory cells (1 mark)
- The second dose produces antibodies (in secondary immune response) in higher concentration and quickly OR The first dose must be small so the animal is not killed (1 mark)
Comments from mark scheme
- Accept in context of primary or secondary immune response
- Credit specificity if given once in relation to T or B cell
- Accept “clone” for “reproduce by mitosis”
- “Clonal selection of B cells” = mp1
- Accept “a lot of antibody” for “higher concentration of antibody”
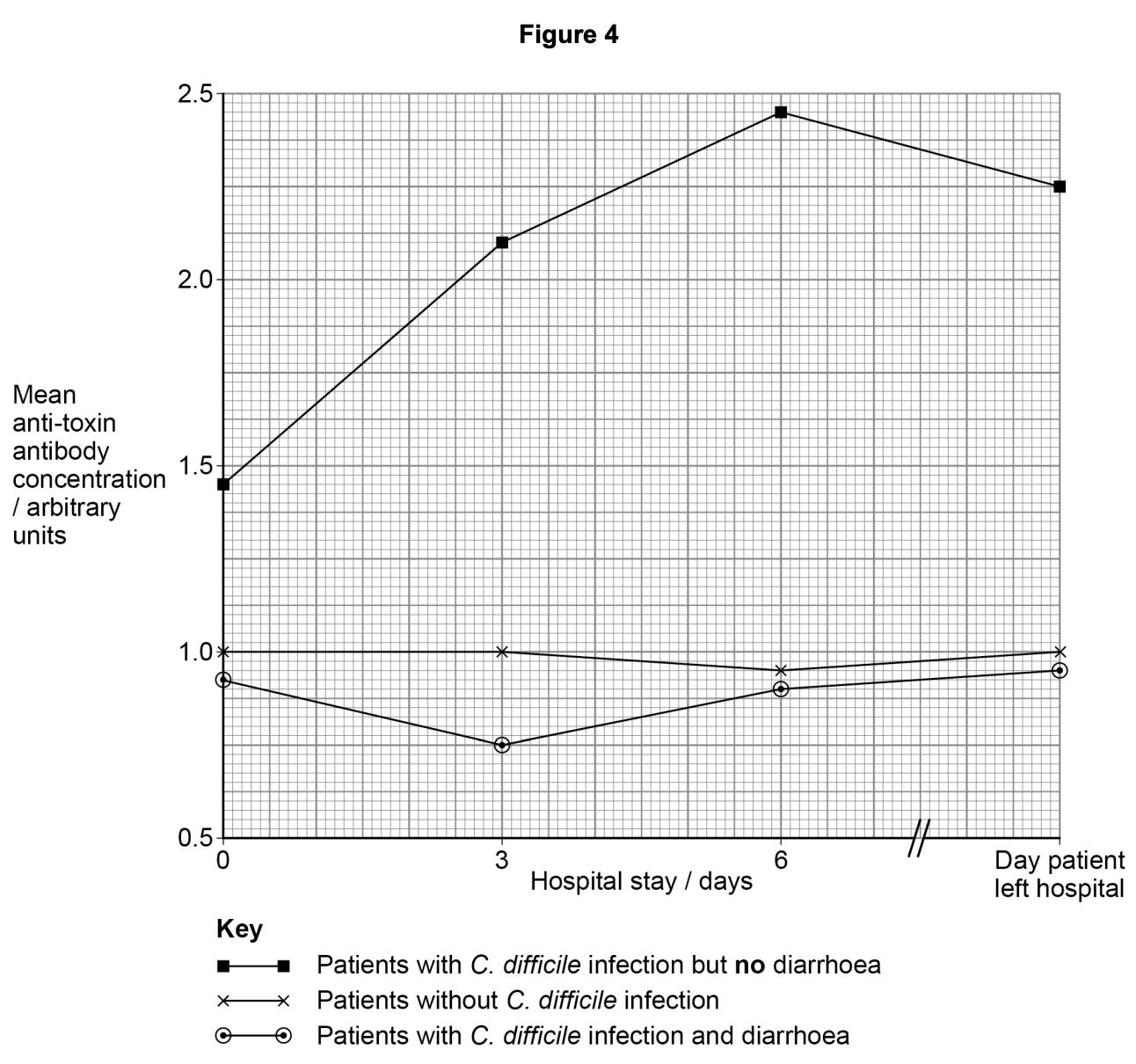
Not all patients in hospital with C. difficile develop diarrhoea. Scientists measured the anti-toxin antibody concentration in hospital patients with and without C. difficile infection. They measured the anti-toxin antibody concentration four times:
- on admission to hospital (day 0)
- on day 3
- on day 6
- on the day the patient left the hospital.
Figure 4 shows the scientists’ results. The scientists suggest that the anti-toxin antibody could be given to some patients as a form of passive immunity.
Use Figure 4 to suggest how this passive immunity would work and which patients should be offered this anti-toxin antibody.
Hint
This is about passive immunity and toxins, not active immunity or pathogens. How do antibodies neutralise toxins?
Mark Scheme
- Anti-toxins/antibodies cause phagocytosis / destruction / agglutination / neutralisation (of toxin) (1 mark)
- Anti-toxin/antibody prevents/reduces (chance of) diarrhoea OR (C. difficile) patients with no diarrhoea have high(est) (concentration of) anti-toxin/antibody OR (C. difficile) patients with diarrhoea have low(est) (concentration of) anti-toxin/antibody (1 mark)
- (Offered to C. difficile) patients with diarrhoea OR (Offered to) patients with low (concentrations of) anti-toxin/antibody (1 mark)
Comments from mark scheme
- For “neutralised”, accept idea of preventing toxin binding/damaging cells lining the ileum
- Accept “people” for “patients”
- Ignore “symptoms” for “diarrhoea”
- Accept “passive immunity offered” for “antibody offered”
Tips from examiner reports
- Passive immunity involves antibodies given directly, not produced by the body’s own immune system
- Antibodies neutralise toxins — don’t say they “destroy the pathogen” when the question is about anti-toxin
- Don’t write a general description of active immunity if the question asks about passive immunity
- Always link your answer to the data provided (Figure 4)
Comments from mark scheme